The workshop was subtitled “The many roles of imaging for a multifaceted disease” and was chaired by Patrick Omoumi, MD, PhD, Head of Musculoskeletal Imaging, Lausanne University Hospital as well as by Julien Favre, PhD, Head of Swiss Biomotion Lab, Lausanne University Hospital. A pre-congress workshop dealt with the topic of biomechanical assessment and included a visit of the Swiss Biomotion Lab (SBML). For the following 2 ½ days, about 100 scientist presented work as key notes, oral presentations, and poster presentations on all topics and across all imaging method used in the field of osteoarthritis.

The PROTO partner from Paracelsus Medical University (PMU), namely members from the “Department for Imaging and Functional Musculoskeletal Research” at the Institute of Anatomy and Cell Biology, gave 5 presentations, mainly focused on the automated measurement of the transverse relaxation time (T2) of articular cartilage using convolutional neural networks (CNNs). These type of measurements are currently developed in the OA-BIO Eurostars-2 project (E! 114932), and will eventually be applied in clinical studies, including the two clinical trials performed within PROTO. The specific purpose of the technique is to track, in addition to cartilage thickness, the compositional and biomechanical properties of the cartilage over time and between different study populations and/or treatments, to which T2 has been shown to be sensitive to. Automization of the segmentation process, which was thus far very labor intensive, will permit scaling these types of MRI-analyses to larger clinical trials at reduced cost and human effort.
Susanne Maschek and co-workers reported on the agreement and precision of femorotibial cartilage T2 at different magnetic field strengths, namely 0.5T, 1.5T, 3.0T, and 7.0T. Whereas the use of 0.5T scanners may permit wider use in clinical practice, the use of 7.0T is potentially interesting in specific research questions that require higher spatial resolution. Yet, with the current systems in use, there were systematic offsets of cartilage T2 between these magnets, and the test-retest precision was greatest at 3.0T.
 Anna Wisser et al. compared fully automated vs. manual image analysis for the assessment of cartilage T2 in knees free of radiographic signs of OA, some with MRI cartilage thickness lesions and some without. She found that the fully automated technology was as discriminatory between both groups as was the manual segmentation, with the superficial cartilage displaying significant T2 differences between knees with and without cartilage lesions, and hence providing strong “clinical validation” of the novel method.
Anna Wisser et al. compared fully automated vs. manual image analysis for the assessment of cartilage T2 in knees free of radiographic signs of OA, some with MRI cartilage thickness lesions and some without. She found that the fully automated technology was as discriminatory between both groups as was the manual segmentation, with the superficial cartilage displaying significant T2 differences between knees with and without cartilage lesions, and hence providing strong “clinical validation” of the novel method.
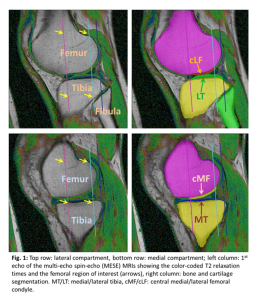
Felix Eckstein and co-workers presented on the cartilage T2 in patients after anterior cruciate ligament (ACL) injury in functional copers, non-copers, ACL-reconstructed patients, and in healthy controls. Particularly, he studied the agreement of automated laminar femorotibial cartilage T2 analysis with that based on manual expert segmentation, and was able to show that the longitudinal increase in deep layer cartilage T2 in the lateral femorotibial compartment in knees with ACL injury was as strong using the automated method compared with the traditional manual segmentation approach.
Finally Wolfgang Wirth and co-workers provided a comprehensive analysis of the semi-quantitative and quantitative imaging biomarker distribution between three endotypes of knee OA that had been previously derived from biomechanical markers, with the analysis including both the APPOACH and the Osteoarthritis Initiative (OAI) Cohort.
The imaging workshop finished on July 1st, with a great day on Lake Geneva and a visit of the opening of the Montreux Jazz Festival.


